Liver Metastases (Secondary Liver Cancer)
Patient’s information
Liver metastases are cancerous tumors that have spread (metastasized) to the liver from another part of the body. These tumors can appear shortly after the original tumor develops, or even months or years later.
The liver
The liver the largest solid organ in the human body. It lies within the tummy on the right side of the ribs, just below the lungs. The liver has two lobes and is further divided into 8 segments.
The liver and bile duct system
Unlike other organs in the human body, the liver’s blood supply is double by two vessels that supply blood, oxygen, and nutrients. The portal vein brings blood from the digestive system and accounts for 70-80% of the liver’s blood supply. The hepatic artery carries 20-30% of blood to the liver. Liver tumors get to take blood supply from branches of the hepatic artery. The liver is your body’s metabolic factory and helps to control more than 500 chemical reactions, including:
Storing carbohydrates
Breaking down proteins
Converting ammonia to urea; a substance found in urine
Using fats to provide energy
Producing cholesterol which is needed for the production of bile (which in turn helps to digest fats in the food) and hormones
Storing minerals and vitamins
Processing blood (breaking down old red blood cells and producing clotting factors).
Secondary liver cancer:
The human body is made up of millions of cells. These cells have different shapes and functions in different parts of the human body. The routine wear & tear of the body cells is controlled by a process called the cell cycle. This process is strictly regulated by the body’s control mechanisms. In cancers, the cells reproduce in an uncontrolled fashion which can lead to the formation of growth or tumor. The cancer cells develop the ability to invade and destroy surrounding cells by a process called invasion and eventually can spread to the other parts of the body (a process called metastases). Some of the cells that form a lump are malignant (cancerous); others are benign (non-cancerous).
More about Secondary liver cancer:
The cells which do not spread to other parts of the body (benign tumors) may cause symptoms as they grow by pressing on the surrounding organs. A lump can be diagnosed as benign or malignant with help of different investigations; such as blood tests, x-rays, ultrasound, and CT scans. Examination of the affected cells under a microscope can confirm the diagnosis of cancer. The special stains & techniques can also help to determine the origin of cancer. This can also tell us whether cancer has started in the area affected (primary) or has spread from another part of your body (secondary).
Most liver metastases start as cancer in the colon or rectum. Up to 70 percent of people with colorectal cancer eventually develop liver metastases. This happens in part because the blood supply from the intestines is connected directly to the liver through a large blood vessel called the portal vein.
Although much less common, liver metastases can also start as breast cancer, esophageal cancer, stomach cancer, pancreatic cancer, lung cancer, kidney cancer, and skin cancer.
Symptoms of Liver Metastases
It can be hard to recognize the symptoms and signs that cancer has spread to your liver. Many people don’t notice anything unusual to indicate that they’ve developed liver metastases. Some say they feel some abdominal discomfort or pain, or have one or more of the following signs or symptoms:
- an overall feeling of weakness and poor health
- loss of appetite
- weight loss
- fever
- fatigue
- bloating
- itching
- swelling of the legs (edema)
- yellowing of the skin or whites of the eyes (jaundice)
Speak with your doctor if you have any of these symptoms so that you can be sure to get a diagnosis and treatment if needed.
Liver Metastases Diagnosis & Staging
To diagnose secondary liver cancer and figure out how far cancer has spread, your doctors may recommend one or more of the following tests:
Clinical evaluation by the doctor to look for the presence of jaundice (yellowness of skin and eyes) or the presence of scar marks (due to itching) and presence of any lumps in the tummy.
Blood tests including LFTs (bilirubin level in your blood will be high due to the blockage of the bile duct).
Hemoglobin (Hb level) can below
Tumor markers. These are substances normally seen in the blood, however, in people with cancer, they may be high. In bile duct cancer, the tumor marker that has been associated with liver metastases are; CEA, Ca125, Ca19.9.
Ultrasound scan
CT scan
MRI (magnetic resonance imaging)
Positron emission tomography (PET) scan: starts with an injection of radioactive sugar. Because cancer cells absorb sugar faster than normal cells, they are highlighted on the PET scan.
Biopsy (histology):
All of the previously mentioned tests may lead the doctor to diagnose liver metastases. However, the only definite way to confirm this diagnosis is to examine some of the abnormal tissue (cancer cells) under a microscope. If a sample of tissue is required we may perform a biopsy. This is when a needle is passed through your skin, into the affected area. If your doctor is planning to treat your cancer with surgery, you may not undergo a biopsy, as tissue confirmation can be obtained after the operation, by the laboratory.
Laparoscopy:
This is a small operation that allows the doctors to look at your gallbladder, liver, and other organs close to the gall bladder. It is done under a general anesthetic and you will have a short stay in hospital. While you are asleep under an anesthetic, the doctor makes a small cut (incision) in your tummy (abdomen). They will insert a thin, flexible tube with a light and camera (laparoscope). They may take a small sample of tissue (biopsy) to look at under a microscope.
After a laparoscopy, you will have one or two stitches in your tummy. You may have uncomfortable wind or shoulder pains for several days after the operation. You can often ease the pain by walking or taking sips of peppermint water.
You may undergo one or more of the scans in order to help identify the tumor and assess your suitability for the various treatments.
Stages of Liver Metastases
Cancer staging is a way of describing how advanced a cancer is, or to what stage it has developed. Because liver metastases have already spread to the liver from somewhere else in the body, they are called stage IV cancer. This is the most advanced stage of cancer. Knowing the stage of cancer helps our experts build a plan of care that fits your unique needs.
Liver Metastases Treatment
Because liver metastases spread to the liver from another part of the body, they can be very difficult to treat. But with the right approach, remission and even a cure are possible for some patients. To build the most effective plan for you, our liver metastases experts carefully consider the latest surgical and interventional radiology techniques, including minimally invasive approaches that often can lessen pain and the time it takes to recover. To customize a treatment approach for you, we’ll want to learn about
- wherein your body the primary cancer is located
- the size and number of liver metastases you have
- your general health
Overall, advances in surgical approaches and treatment strategies have improved the length and quality of life of people diagnosed with liver metastases. Treatment options we can consider include surgery, image-guided interventional therapies, radiation therapy, chemotherapy, and targeted therapy.
Our goal is to provide treatment options that give you the very best possible quality of life and chance for survival.
Surgery for Liver Metastases
When possible, surgeons use techniques that leave more of the healthy liver intact. This reduces the risk of complications and the need for the liver to grow back.
Surgery for People with Colon or Rectal Liver Metastases
For people with liver metastases from tumors in the colon or rectum, liver surgeons can often remove tumors in both places during the same operation. This can be a good approach when there are just a few small tumors in the liver.
Your treatment team often combines this approach with chemotherapy. This approach can significantly reduce complications and recovery time. Studies suggest that up to half of all people who have colorectal liver metastases survive for at least five years after this treatment.
Laparoscopic Surgery
For certain people, minimally invasive laparoscopic surgery can significantly reduce the time it takes to recover from an operation. In this procedure, surgeons insert a thin, lighted tube with a camera on its tip (a laparoscope) through a tiny abdominal incision (cut). The surgeon then guides surgical instruments through the laparoscope to remove tumors or, in some cases, part of the liver.
Ablation to Destroy Liver Metastases
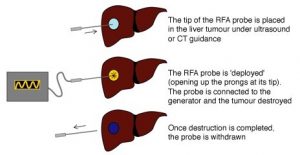
Ablation is a technique for eliminating tumors without surgery. Our radiologists use several forms of energy to select which tumors to ablate. This procedure can be done with minimally invasive techniques on an outpatient basis (no hospital stay needed). Often, our doctors can deliver tumor-eliminating energy through a needle-like probe that they insert through the skin and guide into the tumor with the help of advanced imaging technologies. The most common ablation methods destroy the cancerous tissue through the application of heat delivered by radio waves (radiofrequency ablation) or microwaves (microwave ablation), or through cold gas to freeze the tumor (cryoablation).
Ablation may also reduce the risk of cancer coming back for people with liver metastases that can’t be completely removed. It may prolong survival for people with recurrent metastases whom doctors previously treated with surgery and chemotherapy.
Radioembolization/Selective Internal Radiation Therapy (SIRT)
Selective internal radiation therapy (SIRT), for people who have liver metastases that a surgeon can’t remove, or whose liver metastases are the primary problem. SIRT combines radiation therapy with embolization, which involves injecting tiny particles to block or reduce blood flow to cancer cells. In SIRT, tiny radioactive beads are delivered to the tumor site and trapped there.
Chemotherapy & Targeted Therapy for Liver Metastases
Chemotherapy uses chemical substances to destroy cancer cells wherever they are in the body. This approach can significantly increase the length of life in people with liver metastases. Given before surgery, chemotherapy can lower the risk of tumors coming back later on. Chemotherapy can also help shrink liver metastases from the colon and rectum so that they’re safer for a surgeon to take out.
Targeted Therapies
Chemotherapy drugs destroy some healthy cells in addition to cancer cells. Biologic drugs are more targeted. They can stop tumor cells from replicating and can disrupt the flow of blood to a tumor. Your treatment team may recommend the following biologic drugs to treat liver metastases:
- anti-angiogenesis drugs stop the growth of blood vessels that nourish tumors. Our doctors can give anti-angiogenesis drugs with chemotherapy before or after surgery.
- epidermal growth factor receptor (EGFR) inhibitors block a protein that may contribute to the progression of colorectal cancer.
Before treating you with one of these drugs, your doctor will test you for a mutation in your KRAS gene. EGFR inhibitors aren’t effective when this mutation is present. Clinical trials are underway to evaluate drugs that may be effective in treating patients with a KRAS gene mutation.
Radiation Therapy for Liver Metastases
Radiation therapy can help to control the growth of liver metastases. This approach primarily used for patients when:
- cancer can’t be removed with surgery
- the tumors in the liver are too large for treatment with ablation, a technique done by our interventional radiologists.
Your treatment team will work with specialists from our medical physics department to customize a plan of care that fits your unique needs. This plan includes the latest techniques to deliver radiation directly to the tumor and minimize damage to healthy tissue. Intensity-modulated radiation therapy and stereotactic body radiation are two approaches that can reduce damage to normal tissue being treated for liver metastases:
- intensity-modulated radiation therapy (IMRT) uses radiation beams of varying intensity that mold to the shape of the tumor. Sophisticated software and 3-D images from CT scans enable your doctor to focus radiation on cancerous tissue more precisely.
- stereotactic body radiation therapy uses a highly focused radiation field to deliver larger doses of radiation in fewer treatments. It combines IMRT and image-guided radiotherapy. Your doctor implants tiny markers into the tumor. A CT scan picks up the location of those markers, guiding radiation to the tumor.
Palliative care: If after a detailed discussion of the treatment options you and your family decide rather not to receive any active treatment for your condition, or we feel that active treatment would not help you; the team will refer you for palliative care (supportive care to alleviate symptoms, not a curative treatment) near your home. Supportive care can also be offered to you if you are undergoing treatment such as chemotherapy, which is not expected to offer you a cure.
Follow-up
After your treatment, you will have regular check-ups and possibly scans or x-rays. These may continue for several years. Fighting cancer can be overwhelming. Following surgery or other treatments for metastatic liver cancer, you may notice changes in your strength, flexibility, balance, and endurance. Rehabilitation therapy can help improve your quality of life. Physical therapists work closely with your medical team to design an exercise program that works for you. We offer patients valuable techniques to increase mobility and decrease pain after surgery.
Sometimes, you and your loved ones just need someone to talk to, someone who’s trained to help you make sense of your experience before, during, and after treatment for cancer.
Cancer and its treatment are a challenge for anyone, regardless of age. But if you’re over 65, you may face unique issues that only affect people in your age group. We’re committed to providing cancer patients of all ages with the treatment, facilities, and support they need.
Your treatment team will include healthcare professionals who have the specialized training and experience to effectively treat older patients. Every aspect of your care — diagnosis, treatment, recovery, support — will be tailored to meet your particular needs.
Mr. Touseef Ahmed
0307- 5446668
Transplant Coordinator: (for post-transplant follow up patients):
Mubashar Saeed
0314- 5313905
Hepatobiliary & Pancreatic Surgery Services:
Muhammad Asif 0341-0543883
Qaiser Rafiq John
0321- 4944552
OPD Appointments:
042 36093000
0341-0543883
24 Hours Patients emergency Helpline:
042 111 117 554
Email: info@faisaldar.com
Website: www.faisaldar.com