Neuroendocrine Tumor (Carcinoid Cancer)
Patient’s information
Cancer:
The human body made up of millions of cells. These cells have different shapes and functions in different parts of the human body Carcinoid tumor. The routine wear & tear of the body cells controlled by a process called the cell cycle. This process strictly regulated by the body’s control mechanisms. In cancers, the cells reproduce in an uncontrolled fashion which can lead to the formation of growth or tumor. The cancer cells develop the ability to invade and destroy surrounding cells by a process called invasion and eventually can spread to the other parts of the body (a process called metastases).
Some of the cells that form a lump malignant (cancerous), others benign (non-cancerous). The cells which do not spread to other parts of the body (benign tumors) may cause symptoms as they grow by pressing on the surrounding organs. A lump diagnosed as benign or malignant with help of different investigations, such as blood tests, x-rays, ultrasound, and CT scans. Examination of the affected cells under a microscope can confirm the diagnosis of cancer. The special stains & techniques can also help to determine the origin of cancer.
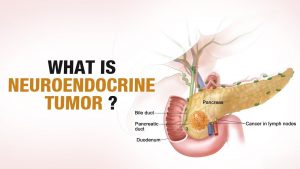
Carcinoid Tumor (Neuroendocrine Tumor)
Carcinoid tumors (also called neuroendocrine tumors or APUDOMAS) the tumors that can develop at any age for no obvious reason. At present nothing known about the cause of these tumors. They do not develop as a result of toxic injury, infections, or drugs, and there no obvious association with any particular lifestyle. Possible causes and include mutations of genes. The primary tumor often develops in the small bowel (small intestine) or appendix but it can occur in many other body parts such as the lung, pancreas, large bowel, ovary, or testis.
Quite often the primary tumor too small and remains hidden and finding and removing the original primary tumor may not necessarily help once metastases (secondary tumors) have occurred. Sometimes the primary tumor diagnosed so early and removed without any spread, but frequently it only diagnosed and once it spread to the liver.
Symptoms of Neuroendocrine (Carcinoid) Tumors:
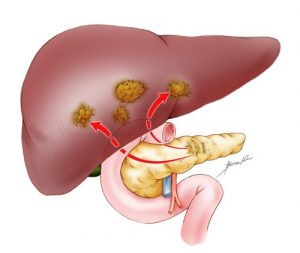
The tumors in the liver are usually multiple and cause the liver to enlarge slowly. which can cause some pain on the right side of the abdomen or in the back.
Some of the carcinoid tumors produce hormones, which chemical substances that generate rather odd symptoms in the body. The “carcinoid syndrome” a combination of variable symptoms where patients develop severe flushing and sometimes wheezing and diarrhea. All these effects are due to a hormone secreted by the tumor within the liver.
A variety of chemical substances can be produced, causing such effects as diabetes, ulcer in the small bowel, or hypoglycemic (low blood sugar) episodes.
The common chemicals (hormones) produced by the tumors: 5HT (Serotonin) – the most commonly produced hormone in carcinoid tumors (causes flushing, wheezing, and diarrhea), Gastrin (causes ulcers, diarrhea), Insulin (causes low blood sugar)
The rarer tumors include:
Glucagon (causes high blood sugar, rashes), Somatostatin, Pancreatic polypeptide and Vasoactive-intestinal peptide.
How to diagnose Neuroendocrine (Carcinoid) Tumors:
Clinical evaluation by the doctor to look for the presence of symptoms and the presence of any lumps in the tummy. These tumors usually diagnosed with the help of scans (ultrasound, CT, MRI) and blood or urine tests.
24-hour urine collections (passing water into a large bottle for 24 hours) and some special blood samples will often detect whether any hormones being produced by the tumor.
Other methods for finding the primary site may include CT scans of the chest, barium studies of the small bowel, or colonoscopy. A colonoscopy a procedure to examine the large bowel (colon) and carried out with a camera-guided tube called a colonoscope. This is a flexible tube about the width of an index finger with a light and a camera in its tip.
Blood tests are repeated to monitor the progress of this disease. One of the tests that have recently appeared is the Chromogranin A level (a chemical measured in the blood). Repeated tests for this chemical may tell us whether the tumor is growing or moving to other areas of the body.
Histology/cytology:
All of the previously mentioned tests may lead the doctor to diagnose carcinoid cancer. However, the only definite way to confirm this diagnosis is to examine some of the abnormal tissue (cancer cells) under a microscope. A tissue sample taken by performing a biopsy. This when a needle is passed through your skin, into the affected area. If your doctor planning to treat your cancer with surgery, you may not undergo a biopsy, as tissue confirmation can be obtained after the operation, by the laboratory.
Depending on the tumor, the original biopsy (tissue sample taken with a needle or taken during surgery) can be reexamined and stained, using a chemical called MIB-1 stain (or ki67) and this can give an idea of how aggressive the tumor likely to be in the future.
These tumors usually grow slowly so many people do not experience any change to their tumors even over many years.
During your treatment:
you will see many different specialists including gastroenterologists hepatologists oncologists nuclear medicine physicians endocrinologists radiologists. Though these tumors rare, these specialists will see them frequently and so best placed to treat you. They will meet to discuss your case, either in the clinic or separately.
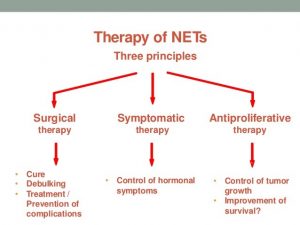
Many different treatment options available to you, including doing nothing. It important to know that some patients will be symptom-free for many years without any treatment. Treatment options include:
Pain medications: simple pain relief, as and when required.
Octreotide injections:
These are normally given once every two or four weeks. These more convenient than twice or thrice daily injections.
Hepatic artery embolization (TAE):
This a procedure done in the x-ray department where a catheter passed into an artery in your leg and threaded up into your liver. A substance then injected in order to block the main artery to the liver. This very effective but can cause pain and produce fevers for some days after the procedure. Occasionally there can be more serious side effects such as liver failure or abscess formation.
Trans-arterial chemo-embolisation (TACE):
TACE (or chemoembolization) sometimes given through the catheter at the same time as the embolization.
Trans-arterial radio-embolization (TARE):
TARE in exactly the same as TACE and with the same aim, but with a radioactive isotope (small radiation-emitting particle) instead of a chemotherapy drug. It will be offered to the patients if it not appropriate to use a chemotherapy drug.
Other more invasive treatments include surgery on the liver (removing one or more secondary tumors from the liver), removing the primary site by surgery, and liver transplantation.
Chemotherapy:
with intravenous drugs, a further option and can be effective in certain types of tumors. Side effects of chemotherapy often nausea, vomiting, skin rashes, and diarrhea. Some, but not all, types will cause hair loss.
In general, pancreatic tumors seem rather more responsive to chemotherapy than those arising from the small bowel or ileum.
More experimental treatments currently being developed. They are forms of targeted radiotherapy (delivering high doses of radiation to the tumors by the “magic bullet principal”). These may be referred to as MIBG therapy, Indium or Yttrium-octreotide therapy. These work by delivering a dose of radiation to the body which can result in temporary damage to the bone marrow. You will need to have regular blood tests to monitor this. The radiation may also affect your kidneys and occasionally it can cause infertility.
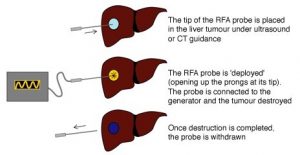
Radiofrequency ablation (RFA):
A form of treatment that consists of putting needles or probes through the skin directly into the tumor and passing some radiation through the tumor. This done under local or general anesthetic.
Alcohol ablation:
has also been injected into these tumors with a needle through the skin and this can reduce the size of the tumor in some cases.
Palliative care:
If after a detailed discussion of the treatment options you and your family decide. rather not to receive any active treatment for your condition, or we feel that active treatment would not help you. the team will refer you for palliative care (supportive care to alleviate symptoms, not a curative treatment) near your home. Supportive care can also offered to you if you undergoing treatment such as chemotherapy, which not expected to offer you a cure.
Transplant coordinator:
Mr. Touseef Ahmed
0341 0543883
0307 5446668
Opd appointments
042 111 117 554
042 36093000
Email: info@faisaldar.com